Highlights

Blood Thinners: Using Them Safely
About Your Blood Thinner Your doctor has prescribed a medicine called a blood thinner to prevent blood clots. Blood clots can put you at risk for heart attack, stroke, and other serious medical problems. A blood thinner is a kind...
Botulinum Toxin for Focal Dystonia
Botulinum injections often are the most effective treatment for the focal dystonias. Injections of small amounts of this chemical into affected muscles prevent muscle contractions and can provide temporary improvement in the abnormal postures and movements that characterize dystonia. First used...
Caregiving a Parent with Alzheimer's Disease
Alzheimer's disease is an illness of the brain. It causes large numbers of nerve cells in the brain to die. This affects a person's ability to remember things and think clearly. People with AD become forgetful and easily confused. They may...
Disease-Modifying Treatments for MS
Current therapies approved by the U.S. Food and Drug Administration (FDA) for MS are designed to modulate or suppress the inflammatory reactions of the disease. They are most effective for relapsing-remitting MS at early stages of the disease. Injectable medications...
Electromyogram (EMG)
What are electromyography (EMG) and nerve conduction studies? Electromyography (EMG) and nerve conduction studies are tests that measure the electrical activity of muscles and nerves. Nerves send out electrical signals to make your muscles react in certain ways. As your...
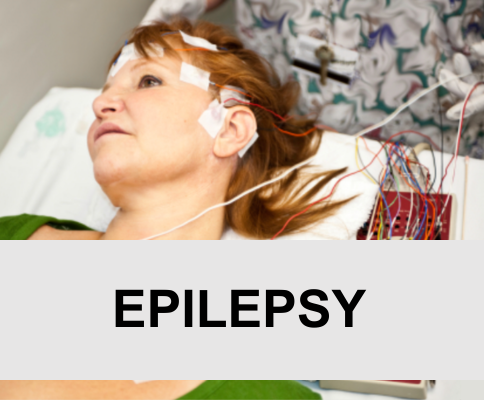
Epilepsy - Driving and Recreation
Epilepsy and Driving Most states and the District of Columbia will not issue a driver's license to someone with epilepsy unless the person can document that she/he has been seizure-free for a specific amount of time (the waiting period varies...
First Aid for Seizures
What should I do if I see someone having a seizure? If you see someone having a seizure with convulsions and/or loss of consciousness, here's how you can help: Roll the person on his or her side to prevent choking...
Headache Diary
Keeping a headache diary can help a physician better diagnose your type of headache and determine the best treatment. Download the HEADACHE DIARY (PDF). After each headache, note the time of day when it occurred; its intensity and duration; any...

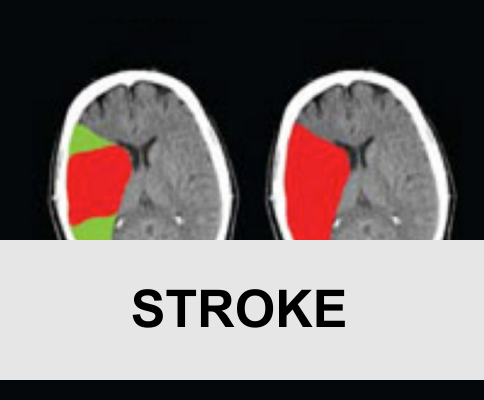
Recommended
Cluster Headache at Neurology Associates, P.C.
Definition of Cluster Headache A cluster headache is one of the most painful types of headache. A striking feature of cluster headache is that the attacks occur in cyclical patterns, or clusters — which gives the condition its name. Bouts of...
Definition of Transient Global Amnesia at Neurology Associates, P.C.
Definition of Transient Global Amnesia Transient global amnesia is a sudden, temporary episode of memory loss that can't be attributed to a more common neurological condition, such as epilepsy, transient ischemic attack, stroke or head injury. During an episode of transient global amnesia, your recall of recent events...
Essential Tremor at Neurology Associates, P.C.
Essential tremor can affect almost any part of your body, but the trembling occurs most often in your hands — especially when you try to do simple tasks, such as drinking a glass of water, tying your shoelaces, writing or shaving....
Meralgia Paresthetica at Neurology Associates, P.C.
Definition of Meralgia Paresthetica Meralgia paresthetica is a condition characterized by tingling, numbness and burning pain in the outer part of your thigh. The cause of meralgia paresthetica is compression of the nerve that supplies sensation to the skin surface of...
Multiple Sclerosis at Neurology Associates, P.C.
Definition of Multiple Sclerosis Multiple sclerosis (MS) is a potentially debilitating disease in which your body's immune system eats away at the protective sheath that covers your nerves. This interferes with the communication between your brain and the rest of your body. Ultimately,...
Parkinson's Disease at Neurology Associates, P.C.
Definition of Parkinson's Disease Parkinson's disease develops gradually, often starting with a barely noticeable tremor in just one hand. But while tremor may be the most well-known sign of Parkinson's disease, the disorder also commonly causes a slowing or freezing...
Post-concussion Syndrome at Neurology Associates, P.C.
Definition of post-concussion syndrome Post-concussion syndrome is a complex disorder in which concussion symptoms — such as headaches and dizziness — last for weeks and sometimes months after the impact that caused the concussion. Concussion is a type of mild traumatic brain...
Rebound Headache at Neurology Associates, P.C.
Definition of Rebound Headache You feel a headache coming on, so you reach for a pain reliever. Or maybe you take pain medication in advance — even every day — to stave off frequent headaches. After all, that's what pain relievers are...
Thoracic Outlet Syndrome at Neurology Associates, P.C.
Definition of Thoracic Outlet Syndrome Thoracic outlet syndrome is a group of disorders that occur when the blood vessels or nerves in the thoracic outlet — the space between your collarbone (clavicle) and your first rib — become compressed. This can...
Trigeminal Neuralgia at Neurology Associates, P.C.
Trigeminal neuralgia is a chronic pain condition that affects the trigeminal nerve, which carries sensation from your face to your brain. If you have trigeminal neuralgia, even mild stimulation of your face — such as from brushing your teeth or putting...
