 A sprain is a stretch and/or tear of a ligament (a band of fibrous tissue that connects two or more bones at a joint). One or more ligaments can be injured at the same time. The severity of the injury will depend on the extent of injury (whether a tear is partial or complete) and the number of ligaments involved.
A sprain is a stretch and/or tear of a ligament (a band of fibrous tissue that connects two or more bones at a joint). One or more ligaments can be injured at the same time. The severity of the injury will depend on the extent of injury (whether a tear is partial or complete) and the number of ligaments involved.
A strain is an injury to either a muscle or a tendon (fibrous cords of tissue that connect muscle to bone). Depending on the severity of the injury, a strain may be a simple overstretch of the muscle or tendon, or it can result from a partial or complete tear.
Causes of Sprains
Sprains usually result from a fall, a sudden twist, or a blow to the body that forces a joint out of its normal position and stretches or tears the ligament supporting that joint. Typically, sprains occur when people fall and land on an outstretched arm, slide into a baseball base, land on the side of their foot, or twist a knee with the foot planted firmly on the ground.
Sprain Locations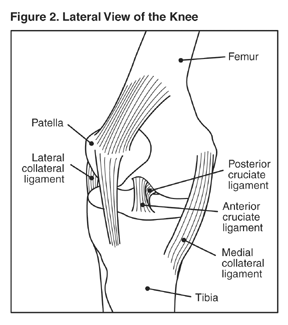
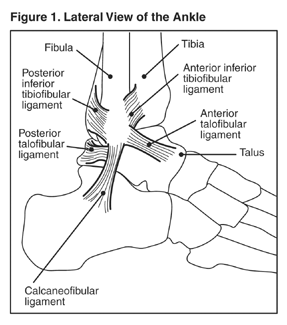
Sprains can occur in any joint, but the the ankle is the joint most commonly sprained.
The ankle joint is supported by several lateral (outside) ligaments and medial (inside) ligaments. Most ankle sprains happen when the foot turns inward as a person runs, turns, falls, or lands on the ankle after a jump. This type of sprain is called an inversion injury.
The knee is another common site for a sprain. A blow to the knee or a fall is often the cause; sudden twisting can also result in a sprain.
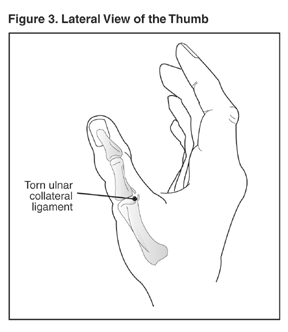
Sprains frequently occur at the wrist, typically when people fall and land on an outstretched hand. A sprain to the thumb is common in skiing and other sports. This injury often occurs when a ligament near the base of the thumb (the ulnar collateral ligament of the metacarpo-phalangeal joint) is torn.
Signs and symptoms of a sprain
 The usual signs and symptoms include pain, swelling, bruising, instability, and loss of the ability to move and use the joint (called functional ability). However, these signs and symptoms can vary in intensity, depending on the severity of the sprain. Sometimes people feel a pop or tear when the injury happens.
The usual signs and symptoms include pain, swelling, bruising, instability, and loss of the ability to move and use the joint (called functional ability). However, these signs and symptoms can vary in intensity, depending on the severity of the sprain. Sometimes people feel a pop or tear when the injury happens.
Doctors closely observe an injured site and ask questions to obtain information to diagnose the severity of a sprain. In general, a grade I or mild sprain is caused by overstretching or slight tearing of the ligaments with no joint instability. A person with a mild sprain usually experiences minimal pain, swelling, and little or no loss of functional ability. Bruising is absent or slight, and the person is usually able to put weight on the affected joint.
When should I see a doctor for a sprain?
- You have severe pain and cannot put any weight on the injured joint.
- The injured area looks crooked or has lumps and bumps (other than swelling) that you do not see on the uninjured joint.
- You cannot move the injured joint.
- You cannot walk more than four steps without significant pain.
- Your limb buckles or gives way when you try to use the joint.
- You have numbness in any part of the injured area.
- You see redness or red streaks spreading out from the injury.
- You injure an area that has been injured several times before.
- You have pain, swelling, or redness over a bony part of your foot.
- You are in doubt about the seriousness of the injury or how to care for it.
A grade II or moderate sprain is caused by further, but still incomplete, tearing of the ligament and is characterized by bruising, moderate pain, and swelling. A person with a moderate sprain usually has more difficulty putting weight on the affected joint and experiences some loss of function. An X-ray may be needed to help the health care provider determine if a fracture is causing the pain and swelling. Magnetic resonance imaging is occasionally used to help differentiate between a significant partial injury and a complete tear in a ligament, or can be recommended to rule out other injuries.
People who sustain a grade III or severe sprain completely tear or rupture a ligament. Pain, swelling, and bruising are usually severe, and the patient is unable to put weight on the joint. An X-ray is usually taken to rule out a broken bone. When diagnosing any sprain, the provider will ask the patient to explain how the injury happened. He or she will examine the affected area and check its stability and its ability to move and bear weight.
What causes a strain?
A strain is caused by twisting or pulling a muscle or tendon. Strains can be acute or chronic. An acute strain is associated with a recent trauma or injury; it also can occur after improperly lifting heavy objects or overstressing the muscles. Chronic strains are usually the result of overuse: prolonged, repetitive movement of the muscles and tendons.
Where do strains usually occur?
Two common sites for a strain are the back and the hamstring muscle (located in the back of the thigh). Contact sports such as soccer, football, hockey, boxing, and wrestling put people at risk for strains. Gymnastics, tennis, rowing, golf, and other sports that require extensive gripping can increase the risk of hand and forearm strains. Elbow strains sometimes occur in people who participate in racquet sports, throwing, and contact sports.
What are the signs and symptoms of a strain?
Typically, people with a strain experience pain, limited motion, muscle spasms, and possibly muscle weakness. They can also have localized swelling, cramping, or inflammation and, with a minor or moderate strain, usually some loss of muscle function. Patients typically have pain in the injured area and general weakness of the muscle when they attempt to move it. Severe strains that partially or completely tear the muscle or tendon are often very painful and disabling.
Treatment of Sprains and Strains
Reduce swelling and pain
Treatments for sprains and strains are similar and can be thought of as having two stages. The goal during the first stage is to reduce swelling and pain. At this stage, health care providers usually advise patients to follow a formula of rest, ice, compression, and elevation (RICE) for the first 24 to 48 hours after the injury. The provider may also recommend an over-the-counter or prescription nonsteroidal anti-inflammatory drug, such as aspirin or ibuprofen, to help decrease pain and inflammation.
For people with a moderate or severe sprain, particularly of the ankle, a hard cast may be applied. This often occurs after the initial swelling has subsided. Severe sprains and strains may require surgery to repair the torn ligaments, muscle, or tendons.
It is important that moderate and severe sprains and strains be evaluated by a health care provider to allow prompt, appropriate treatment to begin. This box lists some signs that should alert people to consult their provider. However, a person who has any concerns about the seriousness of a sprain or strain should always contact a provider for advice.
RICE therapy
- Rest. Reduce regular exercise or activities of daily living as needed. Your health care provider may advise you to put no weight on an injured area for 48 hours. If you cannot put weight on an ankle or knee, crutches may help. If you use a cane or one crutch for an ankle injury, use it on the uninjured side to help you lean away and relieve weight on the injured ankle.
- Ice. Apply an ice pack to the injured area for 20 minutes at a time, 4 to 8 times a day. A cold pack, ice bag, or plastic bag filled with crushed ice and wrapped in a towel can be used. To avoid cold injury and frostbite, do not apply the ice for more than 20 minutes.
- Compression. Compression of an injured ankle, knee, or wrist may help reduce swelling. Examples of compression bandages are elastic wraps, special boots, air casts, and splints. Ask your provider for advice on which one to use, and how tight to safely apply the bandage.
- Elevation. If possible, keep the injured ankle, knee, elbow, or wrist elevated on a pillow, above the level of the heart, to help decrease swelling.
Begin rehabilitation
The second stage of treating a sprain or strain is rehabilitation, whose overall goal is to improve the condition of the injured area and restore its function. The health care provider will prescribe an exercise program designed to prevent stiffness, improve range of motion, and restore the joint's normal flexibility and strength. Some patients may need physical therapy during this stage. When the acute pain and swelling have diminished, the provider will instruct the patient to do a series of exercises several times a day. These are very important because they help reduce swelling, prevent stiffness, and restore normal, pain-free range of motion. The provider can recommend many different types of exercises, depending on the injury. A patient with an injured knee or foot will work on weight-bearing and balancing exercises. The duration of the program depends on the extent of the injury, but the regimen commonly lasts for several weeks.
Another goal of rehabilitation is to increase strength and regain flexibility. Depending on the patient's rate of recovery, this process begins about the second week after the injury. The provider will instruct the patient to do a series of exercises designed to meet these goals. During this phase of rehabilitation, patients progress to more demanding exercises as pain decreases and function improves.
The final goal is the return to full daily activities, including sports when appropriate. Patients must work closely with their health care provider or physical therapist to determine their readiness to return to full activity. Sometimes people are tempted to resume full activity or play sports despite pain or muscle soreness. Returning to full activity before regaining normal range of motion, flexibility, and strength increases the chance of reinjury and may lead to a chronic problem.
The amount of rehabilitation and the time needed for full recovery after a sprain or strain depend on the severity of the injury and individual rates of healing. For example, a mild ankle sprain may require up to 3 to 6 weeks of rehabilitation; a moderate sprain could require 2 to 3 months. With a severe sprain, it can take up to 8 to 12 months to return to full activities. Extra care should be taken to avoid reinjury.
Prevention of sprains and strains
There are many things people can do to help lower their risk of sprains and strains:
- Avoid exercising or playing sports when tired or in pain.
- Maintain a healthy, well-balanced diet to keep muscles strong.
- Maintain a healthy weight.
- Practice safety measures to help prevent falls (for example, keep stairways, walkways, yards, and driveways free of clutter; anchor scatter rugs; and salt or sand icy patches in the winter).
- Wear shoes that fit properly.
- Replace athletic shoes as soon as the tread wears out or the heel wears down on one side.
- Do stretching exercises daily.
- Be in proper physical condition to play a sport.
- Warm up and stretch before participating in any sports or exercise.
- Wear protective equipment when playing.
- Run on even surfaces.
Source: National Institute of Arthritis and Musculoskeletal and Skin Diseases
Last updated : 5/13/2022