Recommended
Acne in Adults
Acne during adulthood is very common. Adult acne can be a continuation of teenage acne that never ended. This is called "persistent acne". It can appear for the first time in people who are 30, 40 or even 50 years...
Actinic Keratoses (AKs)
Actinic keratoses (AKs) are dry, scaly patches that form on sun exposed areas of the skin, including the scalp, face, forearms, and back of the hands. A single lesion is called an "actinic keratosis" or "solar keratosis". Actinic keratoses are...
Actinic Keratoses Treatment Options
What treatment is best for you? What are actinic keratoses? ▪ AKs are rough, dry, scaly patches or growths that form on the skin. ▪ AK’s are considered precancerous lesions cause by UV light (sunlight or tanning booth exposure). ▪...
Advanced Bleaching / Fade Cream
This cream has several key ingredients that work together to “bleach” or lighten dark spots. This is a cosmetic product that is not covered by insurance. Directions Use it twice daily for only 2 continuous months. Key Ingredients Retinoic...
Atopic Dermatitis
Atopic dermatitis (AD) is a chronic skin disorder that causes dry, itching, and inflamed skin. The rash of atopic dermatitis comes and goes. The term eczema is sometimes used to describe atopic dermatitis. Eczema refers to inflamed, itching skin from...
Atopic Dermatitis Treatment
WHAT IS ATOPIC DERMATITIS? Common skin disease affects 10-20% of children and 1-3% adults Multiple names (“eczema,” “dermatitis,” “atopic eczema”) History of asthma, hay fever, allergic rhinitis, or sinusitis SYMPTOMS Itchy, dry, scaly skin that can blister, ooze and weep...
Decubitus Ulcers (Bed Sores)
A decubitus ulcer is an area of skin that breaks down when you stay in one position for too long without shifting your weight. Decubitus ulcers are also called "pressure ulcers" or "bed sores". This often happens if you use...
Drysol Instructions
WEEK 1: – Apply nightly to clean, dry affected area (underarms, palms, or soles). – Cover with plastic wrap for 20 minutes or as tolerated. – Then take plastic wrap off after 20 minutes and throw away. Leave residual drysol...
Hair Loss Treatment
TYPES OF HAIR LOSS ANDROGENIC ALOPECIA: MOST COMMON cause of hair loss in the US is hereditary. TELOGEN EFFLUVIUM: stressors, pregnancy, illness, medications. ALOPECIA AREATA: immune system attacks the hair follicles. OTHER: Anemia Thyroid disease Lupus Menopause Polycystic Ovarian Syndrome...
Indoor Tanning Risks
Indoor Tanning is Dangerous There is compelling, irrefutable scientific evidence which shows that indoor tanning beds can increase your risk for skin cancer. Yet as the evidence of cancer risk grows, more than one million Americans continue to use indoor...
Lamisil Guide
How to Use Terbinafine (Lamisil) 28 day treatment We will write you a prescription for 28 days of treatment BUT you are only using it for 1 week each month. Do not fill the prescription until you follow the steps...

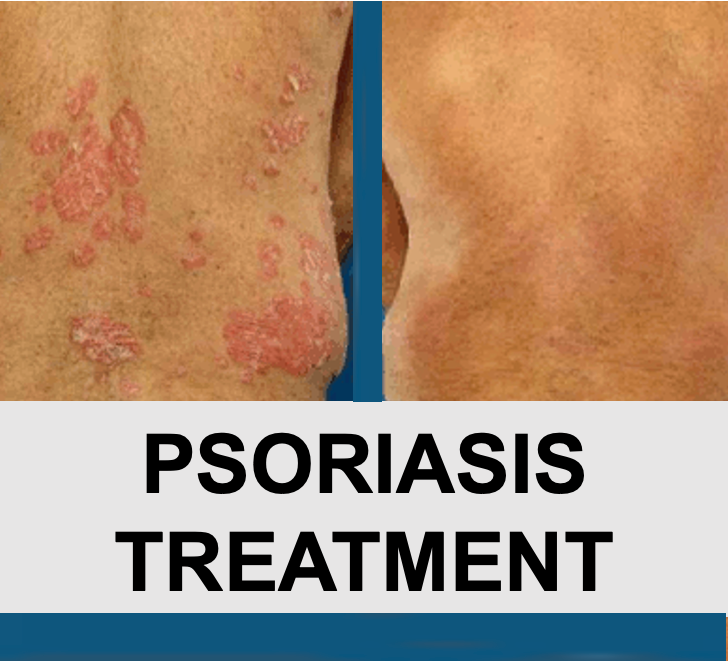
Psoriasis - Questions to Ask
Getting answers to the following questions at your appointment will help prepare you for managing your psoriasis. What type of psoriasis do I have? How severe is it? What are my treatment options and what can I expect from them?...
Qbrexza
What is Qbrexza? Qbrexza (glycopyrronium) cloth towelette is a prescription anticholinergic medicine that is used on the skin to treat excessive underarm sweating in adults and is FDA approved for children 9 years and older. How does Qbrexza work? Glycopyrronium,...
Rosacea Subtype 2 (Bumps & Pimples)
Rosacea can vary substantially from one patient to another. The following photographs reflect common patterns of signs and symptoms, known as subtypes, and many patients have characteristics of more than one subtype at the same time. Papulopustular Rosacea In addition...

Wart Treatment
Warts are caused by the Human Papillomavirus (HPV). Warts are contagious by skin-to-skin contact or by sharing personal items like towels or razors. Genital warts are spread by skin-to-skin or mucosal contact. IN-OFFICE TREATMENT CRYOTHERAPY Liquid nitrogen -196°C is more...
Warts
Warts are growths on the skin caused by the human papillomavirus (HPV). They are very common, particularly in school-age children. Warts can spread by direct contact to other parts of the body, or to others. They are painless unless they...